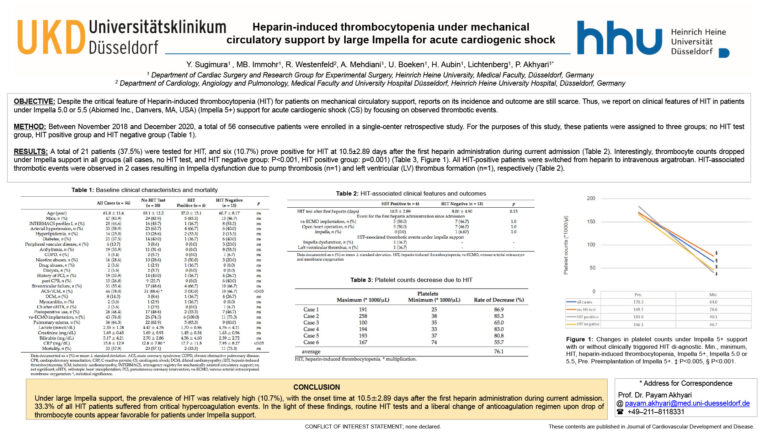
LV Unloading using Imepella Reduces LA Pressure and Volume Overload in Chronic Mitral Regurgitation
Kiyotake Ishikawa, Shin Watanabe, Lauren Leonardson, Kenneth Fish, Roger J Hajjar
Abstract
Mitral regurgitation is a common presentation in patients administered due to the decompensated chronic heart failure. Whether an LV-to-aorta pLVAD can be effective in relieving LA overload remains unclear. LV unloading using an Impella CP reduces LA pressure and volume by actively pumping the blood towards forward direction. Chronic heart failure with mitral regurgitation was induced in Yorkshire pigs (n=3, 20 Kg) by percutaneously severing chordae tendinae of the mitral apparatus with a biopsy catheter. Three months later (body weight 43.5 ± 5.0 Kg), the animals underwent LV unloading with an Impella CP with a maximal flow support (p8). Hemodynamics before and during the LV unloading were assessed by Swan-Ganz catheter and pressure volume loop catheter (Millar catheter) in both LA and LV. Additionally, LA volumes were assessed by 3-dimensional echocardiography before and during the Impella support. At 3 months, animals presented with moderate mitral regurgitation (regurgitant fraction 38±10%) with dilated LV (LV end-diastolic volume: 45.5±1.7 mL to 89.7±18.0, P=0.04, LV end-systolic volume: 12.5±1.6 mL to 31.2±10.9, P=0.10, Day0 to 3 month, respectively). LV unloading resulted in a significant reduction of LV end-diastolic pressure (13.6±2.6 to 4.0±4.0 mmHg, P=0.029). Although the visual assessment of MR degree by color-Doppler echocardiography did not change by LV unloading, mean LA pressure decreased significantly (12.3±7.1 to 9.3±6.1 mmHg, P=0.035). LA v-wave, which is accentuated in the mitral regurgitation due to the regurgitant flow, also reduced significantly, indicating a reduction of quantitative MR (17.3±11.2 to 12.3±9.5 mmHg, P=0.038). Furthermore, maximum LA volume assessed by three-dimensional echocardiography was significantly decreased (46.6±13.4 to 29.7±15.9 ml, P=0.043). LV-to-aorta pLVAD can alleviate LA pressure and volume overload in a heart failure due to mitral regurgitation.